Glenohumeral Arthritis
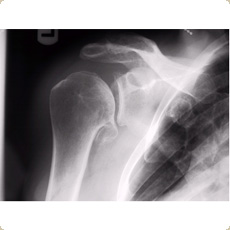
Gleno-humeral arthritis
Arthritis is a condition where the articular cartilage on either side of the glenohumeral joint has worn away. The articular cartilage can be destroyed through the normal wear and tear and aging process but can also occur as a result of inflammatory conditions such as rheumatoid arthritis. Furthermore arthritis can also occur secondary to injury and fractures involving the articular surfaces of the shoulder joint. This is known as post traumatic arthritis. In elderly individuals who have a rotator cuff deficient shoulder the humeral head (ball of the shoulder joint) migrates upwards resulting in rotator cuff arthropathy (arthritis in association with a rotator cuff tear)
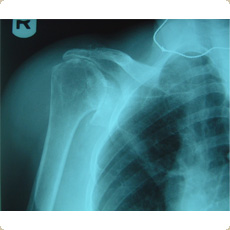
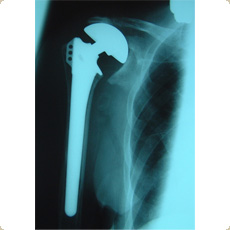
Bipolar Hemiarthroplasty for cuff arthropathy
Longstanding instability of the shoulder and conditions that lead to loss of blood supply of the ball of the shoulder joint (avascular necrosis) can result in secondary degenerate changes in the glenohumeral joint resulting in arthritis.
Patients presenting with glenohumeral arthritis have pain, stiffness and loss of function. They often complain of a grating or creaking sensation in the shoulder joint. They experience difficulty with overhead activities and even simple tasks such as dressing and undressing themselves, acts of personal hygiene and bathing and showering are quite limiting. Routine investigations such as x-rays can easily highlight the classic features of arthritis. In early stages physiotherapy may be beneficial and temporary relief may be achieved through local anaesthetic and steroid injections. The long term use of corticosteroid injections however is detrimental and can actually result in further loss of articular cartilage. In end stage disease then surgery may be considered. Short term relief can be obtained through keyhole surgery to achieve a debridement and washout of joint but a permanent solution may require shoulder replacement surgery either in the form of hemi-arthroplasty in which case only the ball side of joint is resurfaced or a total shoulder replacement where both articulating surfaces are replaced
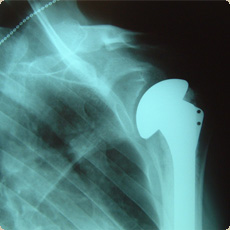
Hemiarthroplasty for gleno-humeral OA
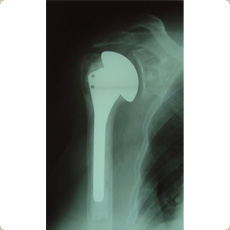
Total Shoulder Replacement
A shoulder resurfacing procedure is a type of shoulder replacement but this is a relatively bone-preserving operation in which the humeral head is smoothed and then is covered with a metal cap. Shoulder replacement surgery requires in-patient stay of up to 5 days. Following surgery an intensive rehabilitation programme is required with the help of the physiotherapists. The patient is required to use a sling for up to two weeks, which is then weaned off over the course of the next 2-4 weeks. The patient is allowed to carry out light manual activities approximately 2-4 weeks after surgery. Driving is generally possible at around the 6 week point. Heavy lifting however is not recommended up to 3 months. The main indication for surgery in individuals with osteoarthritis is pain relief and the overall success is about 85-90%. Generally the range of shoulder motion improves following shoulder replacement surgery but there is always a limitation in terms of the range of shoulder motion achieved. Functional improvement continues up to 18-24 months following surgery.
Documentation
Pre-op Information PackShoulder Physio Protocols
- Arthroscopic Bankart Repair/Mini Open Bankart/Arthroscopic SLAP Repair: Rehabilitation Protocol
- Copeland Shoulder – Resurfacing Arthroplasty: Rehabilitation Protocol
- Arthroscopic Subacromial decompression and/or AC joint excision (partial/no cuff tear): Rehabilitation Protocol 1
- Arthroscopic Acromioplasty (Sub Acromial Decompression) with Rotator Cuff Repair (small/medium tears): Rehabilitation Protocol 2
- Open Acromioplasty ( Sub Acromial Decompression) with Rotator Cuff Repair (large tears): Rehabilitation Protocol 3
- Reverse shoulder replacement (delta3): Rehabilitation Protocol
- Manipulation under anaesthesia and/or Arthroscopic Capsular release of shoulder joint: Rehabilitation Protocol
Contact Us Directly
Sarah Morris, Secretary to Mr PimpalnerkarReferral forms to download:

